Cervical osteoarthritis causes protrusions, ligament thickening, and bony prominences that can narrow the spinal canal through which the spinal cord passes, leading to inflammation or cervical myelopathy.
All connections from the brain to the arms and legs pass through the spinal cord, responsible for sensation, muscle strength, pain and temperature perception, and proprioception. It is a very delicate structure, and spinal cord injuries must be treated early, as no cure has yet been discovered and they leave significant sequelae.
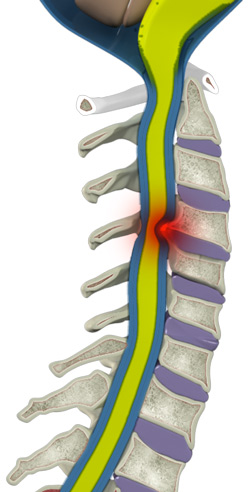
In many patients undergoing cervical MRI, canal stenosis is reported, but not all will develop myelopathy. Therefore, it is very important not to be alarmed and to consult with a spine specialist who can clarify your concerns and assess your risk.
How Do I Know If I May Have Cervical Myelopathy?
Cervical stenosis, when affecting the spinal cord, causes a series of symptoms that I have classified according to their severity:
| MILD | MODERATE | SEVERE | |
| HAND MOBILITY | can button clothing but has difficulty manipulating small objects, opening jars, writing a note… | great difficulty buttoning clothing but can eat with a spoon | cannot use a spoon properly loss of hand mobility |
| LEG MOBILITY | moderate imbalance when standing or walking but able to climb stairs without holding the handrail and does not require external aids | walks without a cane/walker but needs to hold the handrail to climb stairs. walks with aids on level ground. | cannot walk and has no sensation in the legs |
| HAND SENSATION | moderate loss of sensation in hands | severe loss of sensation in hands or pain | complete loss of sensation in hands |
| URINARY FUNCTION | urinary urgency (having to rush to the bathroom to prevent urine leakage) or less than one episode per month of stress incontinence. | more than one episode per month of stress incontinence (urine leakage when coughing, sneezing, or with exertion that did not occur previously) | unable to urinate spontaneously, only with catheterization. |
These symptoms appear progressively; that is, it is normal to first experience some of the mild symptoms before feeling the moderate and severe ones. As osteoarthritis progresses, the spinal cord suffers more compression and symptoms worsen—that is, there is progression to increasingly impaired hand and leg mobility and urinary incontinence problems.
It is very rare to suddenly be unable to walk or move the hands without having any prior symptoms. It is also very rare for symptoms to appear before age 50.
The progression is often confused with other neurological diseases and is difficult to detect. Generally, these are patients who have had repetitive episodes of neck pain, many with radiation down the arm, because this is a problem fundamentally associated with cervical osteoarthritis.
What Should I Do If I Have Cervical Stenosis?
If cervical canal stenosis is detected, the spine specialist will evaluate your symptoms and request a test called somatosensory evoked potentials. This test involves applying electrical stimulation to peripheral nerves and recording the signal along the spine, brainstem, and somatosensory cortex with electrodes. It does not use needles but may be uncomfortable for some people.
Based on the symptoms, MRI findings, and evoked potential tests, you will be informed of your risk of developing cervical myelopathy.
Cervical myelopathy occurs, as mentioned, due to progressive compression of the spinal cord in the course of osteoarthritis, but when the canal is very narrow, a fall or traffic accident with sudden neck movement can trigger an acute injury.
What Treatment Will Be Recommended?
If your risk is low, it is sufficient to be aware of the symptoms and consult if any appear, undergo specific rehabilitation, and maintain follow-up appointments with your spine surgeon.
If your risk is moderate or high, surgical intervention will be proposed to decompress the canal and free the spinal cord from compression. This surgery is performed via an anterior or posterior approach (front or back of the neck) depending on the anatomical and radiological characteristics of the cervical spine. The goal of surgery is to halt symptom progression and prevent functional deterioration—that is, to maintain arm and leg function and prevent incontinence.
